The pain we choose: polyvagal theory and enduring the suffering
Humbled by the dentist, I've been exploring the role control—and the human nervous system—plays in my relationship to pain and enduring.
I recently went to the dentist for three fillings, and I’ve been in a slight tailspin about my ability to handle pain and discomfort since. (Three fillings?! I know, I know. I have soft teeth, and I hadn’t been in a while, and one was to fix an old filling that was giving me grief. I promise I’ll floss more.).
I grew up lucky; my grandpa was my dentist. Until I was about 14 years old, I actually had zero idea I’d ever received a shot in my mouth because he’d give me that magical numbing gel and then use his giant grandfather hands to stealthily hide the syringes from my view.
Fast-forward to my adult life, in Montana (thousands of miles from his rural Georgia office still covered in its original 60s wallpaper), and I’ve learned needles are not my friend. Ever since the first time I tried to donate blood in high school and passed out after looking at the haunting needle resting in my vulnerable, soft arm, my nervous system has known one thing:
Needles are dangerous, and the best way to survive them is to immediately lose consciousness.
I’ve got three tattoos, two nose piercings, and have received my fair share of shots and blood draws since that first horrifying experience when the Red Cross set up shop in my gym. And I’ve passed out in most of those experiences, unfortunately worrying (and probably annoying) the professionals giving me a septum ring or making sure my iron levels were healthy.
As I sat in the dentist chair, after warning them of my history and preparing to wake up cold and white-faced from my brain sounding the alarm, all I could think was:
“How the fuck do I run ultras with the entire bottom of my feet blistered and chafing like a bullseye around my you-know-what, but I’m sitting here on the edge of consciousness over a few almost-painless needles to the gum?”
I thought about what we endure as ultrarunners—and the joy we get from enduring these things. Now, it’s most often in the form of Type 2 fun, but sometimes, when we’re really centered and lucky, we get that in-the-freaking-moment, blisters-and-chafing-and-all, pure, insane Type 1 joy. It’s nirvana.
We choose to run long, hard miles knowing that the pain is part of the fun, and we feel empowered for taking it on and surviving. Why couldn’t I apply the same principle to pain at the dentist, and similar procedures at large?
What I know all too well—and reminded myself of in the dentist chair—is that it’s not about the pain we experience. It’s about what control we have over that pain.
The waiting in stillness that defied every instinct in my animal body, the attempt to “be cool” and avoid passing out, and the eerie sound of a needle slicing its way through my gums while I lay in attempted paralysis, felt like a greater assault on my being than the last five hours of my first 100-miler.

Realistically, nothing I was going to experience in that dentist chair was any more uncomfortable or threatening than the hill repeats I did the other day. In fact, I’m certain the workout involved more suffering!
But feeling totally powerless to what’s happening to us, especially when it involves discomfort and pain, is not a fun experience. It can actually feel traumatizing. Our bodies are wired to protect us, and overriding their protective programming sends signals akin to emergency sirens.
Polyvagal Theory: Our Bodies’ Brilliant Instincts
Thanks to both my training as a psychotherapist as well as my own long, winding (and never-ending) journey of healing, I’ve learned a lot about the human nervous system. Or, rather, nervous systems. It is FASCINATING.
We all know about “fight or flight,” that protective response that tells us whether the best way out of danger is to run away or put up our fists. But what recent research has revealed—and what I’m incredibly passionate about leveraging as a somatic (body-based), trauma-focused therapist—is that those aren’t our only options.
Rather, over the millions of years we’ve evolved, our nervous system has branched out and created multiple pathways and responses to protect us—to help us survive. This emerging understanding comes from the groundbreaking work of Stephen Porges and is known as Polyvagal Theory. Here’s the nutshell version:
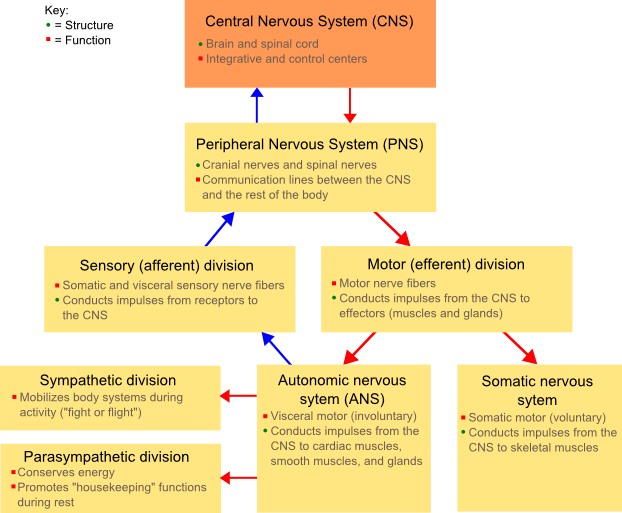
Our central nervous system (the brain and spinal cord) branches into multiple tracks, one of which is the Autonomic Nervous System, or ANS. The ANS controls all our involuntary behaviors, like digestion, heart beat, breathing, and so on. It’s comprised of the sympathetic division and the parasympathetic division. Think of these as the “OFF” and “ON” switches for those housekeeping functions I just listed.
The sympathetic division is the “OFF” switch: When our brain perceives danger, it signals the sympathetic nervous system to shut down all unnecessary functions and instead direct all energy towards mobilizing away from danger, aka, fight-or-flight. (This is why those of us who are often anxious also tend to have stomach discomfort and digestion issues—that part of our system tends to get dampened when our anxiety kicks in.)
The parasympathetic division, on the other hand, is our “ON” switch. When that system is activated, our involuntary bodily functions operate like normal, and we are at ease. The kicker, though, is the way these two branches interact.
In situations where our brain perceives danger (such as a dark alleyway at night, or on a trail run alone in the backcountry, or in, say, a dentist’s chair), it tells our sympathetic branch to come on, mobilizing us to fight or flight. “This is life or death,” it says.
But we don’t always want to let that instinct take over. Maybe if we’re being attacked on the street we do, but what about when we’re finally getting that piercing we’re so excited about, or we need a cavity filled? Our logical brain knows that running out of the piercing shop or punching our dentist in the nose is a bad idea. But our deep, primal nervous system doesn’t.
If we override that sympathetic response to fight or flight, our body brings in the backup. It kicks back to the parasympathetic branch—the one that governs rest and relaxation—and says “Shut it down.” It takes us straight past restful ease. and into full shut-down.
That’s when we pass out. This is the third survival mode: fight, flight, freeze. If you’ve seen animals “play dead,” you’ve seen freeze.
The clinical name for this is vasovagal syncope, the phenomenon where our vagus nerve—and the parasympathetic branch it controls—puts our body in shut-down, or freeze, mode: our blood pressure drops, our heart rate slows, and oxygen to our brain decreases enough that we become distant, dissociated, or even fall unconscious for a brief spell.
It’s our body’s way of saying, “It seems like you’re not able to run or fight your way out of this, so I’m going to do the next best thing I can. I’ll keep you safe.”
It’s what happens to me at piercing shops and doctors offices and the dentist. I deny my natural instinct to get up and leave, or yank the needle away from my face, and my body escalates the alarm, sending me into freeze.
But there is another option: We can learn to recognize these threshold moments and, instead of escalating the alarm, bring ourselves the other direction, back toward baseline and ease.
Knowing what’s happening deep inside, on the primal level we can barely fathom, gives us a little bit of space to shift the things that don’t serve us.
Perhaps that means working, as I have, to show our bodies that even if we are uncomfortable or afraid, they are safe enough to stay present at the doctor or dentist, or in disagreements with our partners, or when we receive bad news.
Mindfulness can be a powerful tool. Because if we recognize that it’s not so much about the pain we’re experiencing, but about our relationship to and control over the pain, then perhaps we can also recognize that we have some choice over how we relate to the pain.
We can practice, one tiny step at a time, enduring the discomfort and offering our inner selves compassion and comfort to start to rewire those patterns that don’t serve us.
Even if the pain wasn’t our choice; even if we’d rather feel anything else (as I would at the dentist), we know what we’re capable of. We know what we’ve endured with a gritty smile on our face and tears of painful joy in our eyes.
If we can remember those moments of triumph over the hurt, maybe we can find it in ourselves to endure the pains that feel less welcome.
This isn’t to say that we can flip a switch in the brain and simply “choose” not to mind the pain. It’s not that simple—the body’s wisdom runs deeper than our conscious cognition—and assuming that is invalidating to so many experiences.
But we can remind ourselves of the strength and endurance we have—that we lean hard into when we choose to pursue a goal that inevitably involves pain and suffering—and we can invite that strength to support us even in the suffering we don’t choose.
In fact, I think that part of why I was able to make it through that appointment without passing out, despite needing seven shots of novocaine, is because of the self-trust and endurance I’ve practiced as an ultrarunner.
Every step, every mile, every triumphant finish line, is a chance to practice moving through suffering, and to show ourselves—the young us, the hurt us, the inner-child us—that we CAN and WILL survive hard things, and we are strong enough to be present for them.
Running is a daily meditation on our resilience, a unique opportunity to show ourselves what we can endure, a repeated experience of survival and triumph—no matter how small.
—Morgan